OUR PATIENT PORTAL IS EXPERIENCING TECHNICAL ISSUES: If you are a current GYN patient using our patient portal, you will not be able to send or receive messages from or to our clinic due to technical difficulties. If you would like to contact us, please reach out via phone at (404) 728-7900. We apologize for any inconvenience this may cause.

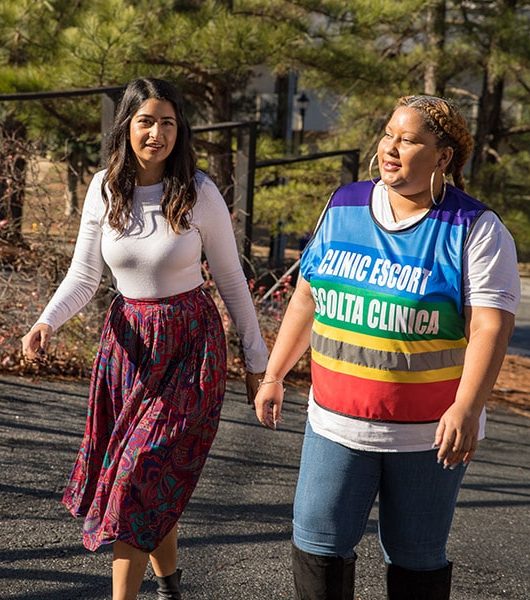


Learn more about our prices and payment options, location and hours, and other appointment details at the link below. Financial assistance is available to those who qualify. Call us at 404-728-7900 to discuss your specific needs.
For over 41 years, Feminist Center, an Abortion Clinic in Atlanta, GA has been providing safe, nonjudgmental and compassionate abortion care services. If you are pregnant and would like to consider your options – we are here to help and will support whatever decision you make.
We provide a wide range of safe and affordable gynecological wellness services including annual exams, STI testing & treatment, birth control, pregnancy testing, etc. We are committed to making our services safe and welcoming to the LGBTQIA+ community.
Since 2000, Feminist Center has offered sensitive, friendly, and affordable health care to transgender, gender non-conforming, and intersex individuals. We currently provide care to trans men, gender non-conforming, and intersex clients from across the Southern states.




Please use this calculator before selecting your options from the appointment form below. Note: Seeing a trained medical professional is the only way to accurately determine the length of your pregnancy and what options are available.
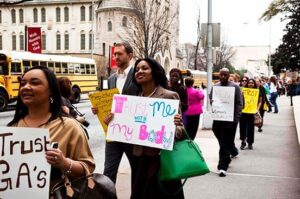


1924 Cliff Valley Way NE
Atlanta, GA 30329
Mon – Fri: 8:00 am to 5:30 pm
Sat: 8:00 am to 2:00 pm
Feminist Women’s Health Center is a 501(c)(3) nonprofit organization | Abortion Clinic Atlanta, GA | EIN 58-1273243 | Powered by Partners For Choice
Feminist Women’s Health Center provides abortion clinic services, abortion pills, gynecologist, birth control services including the IUD, Nexplanon, and the birth control shot to Decatur GA, Scottdale GA, Clarkston GA, Avondale Estates GA, Tucker GA, Stone Mountain GA, Pine Lake GA, Norcross GA, Atlanta GA, Peachtree Corners GA, Lilburn GA, Smyrna GA, Conley GA, Redan GA, Mableton GA, Macon GA, Athens GA, Rome GA, South Fulton GA, Warner Robins GA, Brookhaven GA, Sandy Springs GA, Marietta GA, Dunwoody GA, Stonecrest GA, East Point GA, North Druid Hills GA and College Park Georgia. 2021 Copyright Feminist Women’s Health Center.
If you are pregnant or think you may be pregnant and need an abortion, seek care immediately. We are still providing abortion care up to the legal limit. There are exceptions to the law. Please give us a call to know your options. Read what the 6-week ban means for you.